Health Financing
Why Health Financing is Critical for Universal Health Coverage. Without financial resources, universal health coverage (UHC) – a United Nations Sustainable Development Goal (SDG) emphasizing that everyone should have access to the quality health services they need, and that the use of these services does not expose individuals to undue financial hardship – cannot be achieved. High Performance Health Financing ensures that the resources being used to finance UHC are adequate and sustainable, sufficient to spread risk, as well as efficient and equitable. In this way, high performance health financing also helps to build healthier, more productive populations that can contribute to improved human capital, and in turn, sustainable and inclusive growth.
The focus on effective service coverage and financial risk protection goals under UHC underscores that the way countries finance their health systems matters. Health financing policies address the functions of pooling and purchasing (i.e., how funds are organized and used) and revenue raising (i.e., the level and source of funds), and can help to achieve these goals. In developing countries, domestic public funds – in the form of mandatory, pre-paid and pooled resources – are an essential component of High-Performance Health Financing and progress toward UHC. As such, many policies for high performance health financing in resource limited settings focus on maximizing fiscal space for health through Domestic Resource Use and Mobilization (DRUM), or how domestic resources are mobilized (DRM) and then effectively and efficiently used.1 However, meaningful exchange and dialogue on the “how to” behind policy options is needed in order to move them to action—especially in a post-COVID world where fiscal space is reducing and difficult choices need to be made for prioritization of resources among and within sectors.
The Health Financing Technical Initiative (HFTI). Based on country surveys and responding to a high demand for a technical area on health financing to be part of the JLN’s offering, the HFTI was launched after additional rounds of consultations with JLN member countries and the JLN Steering Group in 2016. Consultations revealed that as countries move towards UHC, their health financing systems are undergoing rapid change and are faced with additional pressures related to transitioning external support, mobilizing domestic resources for health, and efficient allocation of resources given competing priorities. Revisiting conventional financing practices in a peer-to-peer knowledge exchange setting was thus seen as a valuable way forward for countries to gain practical know-how and technical support from each other. To respond to this need, the HFTI made available the following platforms for joint learning:
Institutionalizing Explicit Processes for Setting National Health Priorities - Inactive
National priority setting is an essential step in countries’ strategic planning processes for health. By institutionalizing explicit priority-setting processes for health that are transparent, inclusive, evidence-informed, equitable and accountable, countries can help ensure that health policies, strategies, and plans consistently align with national health and development goals such as UHC, and that scarce human, financial, and other resources are used in a way that is consistent with, and helps to achieve, these goals.
The learning exchange will bring together a group of country representatives with experience in working to institutionalize explicit priority setting as part of strategic planning for the health sector. To learn more, visit the learning exchange page here.
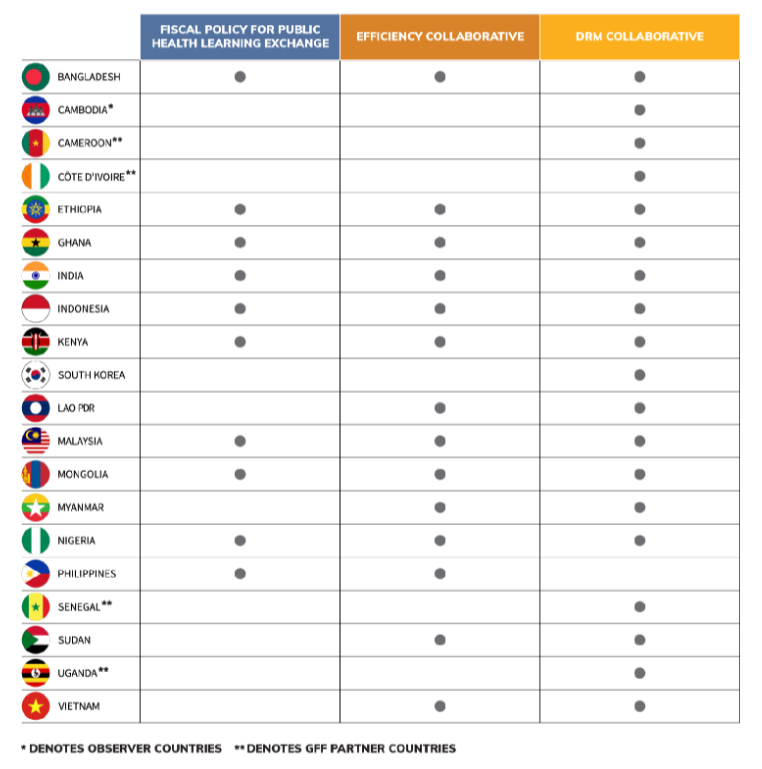
Domestic Resource Mobilization (DRM) collaborative - Active
Since 2017, the DRM collaborative has partnered with the Global Financing Facility (GFF) for a jointly offered learning platform on DRM. With more than 300 participants from the collaborative has facilitated discussions, and shared cross-country knowledge and expertise on pressing questions on DRM for health. The collaborative has worked on co-producing five knowledge products:
- Making the Case for Health: A Messaging Guide
- Dynamic Inventory of DRM Resources and Efforts
- On Prioritizing Health: A Background Analysis
- Policy Dialogue Toolkit
- Narrative Summaries on Public Expenditure for Health
In its second phase of work, the collaborative ihas fostered a community of practice aimed at supporting countries with the adaptation and implementation of the aforementioned knowledge products . The DRM collaborative is also partnering with the Global Financing Facility (GFF) and the (GF) to support in-country application of the knowledge emerging from thecollaborative.
Fiscal Policy for Public Health Learning Exchange - Inactive
This learning exchange was held in February 2018, in Nairobi, Kenya co-located with the third in-person meeting of the Efficiency collaborative – attended by 36 participants from 11 JLN countries. The Fiscal Policy for Public Health Learning Exchange considered positive health outcomes that can be achieved through fiscal policy measures. The overarching objective of this learning exchange was to discuss the use of fiscal policy such as sin taxes for tobacco to discourage consumption and lead to positive health outcomes. This included understanding country experience in feasibility, implementation, achievements and challenges in using fiscal policy for public health, diagnostic tools for evaluating and strengthening tax policies for public health and benefits, political economy, and ease of introduction of tobacco tax. Discussions and key take away messages from the learning exchange were captured in a blog which was published on the JLN website shortly after the event. A report on the learning exchange can be downloaded.
Partnership Initiatives
Annual Health Financing Forum (AHFF) Series. The JLN’s Health Financing Technical Initiative partners annually on the AHFF. The AHFF is focused on health financing resilience during COVID-19 and was held in June and November 2020.
In order to extend the reach and impact of the JLN’s Health Financing Technical Initiative, especially during the COVID-19 pandemic, the World Bank facilitation team leveraged and intensified its existing longstanding collaborations with the World Bank’s Health Financing Global Solutions Group, the Global Financing Facility, and other partners to form a COVID-19 Health Financing Resilience Program.
(Inactive). The Program supports decision-makers to shape health financing policies based on best evidence and emerging lessons by forecasting crisis impact, facilitating knowledge exchange, documenting and analyzing policy responses through a monitoring questionnaire, developing a global research agenda, and revisiting widely accepted policies. A virtual collaboration space has been made available through a community of practice for practitioners to discuss health financing policy responses and their impact and to share country experiences and lessons learned. Launched at the 2020 AHFF, a variety of learning exchanges have since included webinars, roundtables, virtual working groups and facilitated Q&A. Additional resources included a curated repository of technical materials. Members of theJLN Domestic Resource Mobilization (DRM) and Efficiency Collaborative (EC) under the Health Financing Technical Initiative joined as active participants in this expanded community of practice. Additionally, the Health Financing Technical Initiative cross-collaborated as part of the JLN’s new (NODE) to amplify the important intersection of health financing and pandemic response and recovery.
Joint Event with Provider Payment Mechanisms Initiative on Provider Payment in Indonesia, 2017. A facilitated half day learning exchange meeting was held with the Provider Payment Mechanisms Initiative to provide Indonesia with access to peer countries’ experiences in building effective models of strategic health purchasing and financial risk-sharing in decentralized contexts.
 .
.
1 Summarized from Tandon, A. (2020) Global Landscape: Fiscal Space for Health
